Background
In recent years, excessive use of electronic devices has been associated with rising myopia rates among youth in China. By 2020, the number of people with myopia in China was projected to exceed 700 million. The high incidence and decreasing onset age have drawn attention from national authorities, and Chinese media have urged greater emphasis on eye protection and myopia prevention.
Can VR Help Treat Myopia?
Beyond prevention, there is interest in whether methods exist to treat or restore vision for the large population affected by myopia. Virtual reality (VR) technology has been proposed as a possible approach. A recent social media claim that daily VR use improved a user’s vision sparked public debate about whether VR can be therapeutic for myopia and whether there is scientific basis for such claims.
Physiological Basis
Disruption of ciliary muscle function is a major factor in the development of myopia. Prolonged near work reduces the ciliary muscle’s ability to accommodate, and over time axial elongation of the eye can occur, producing myopia. Improving this condition requires strengthening the ciliary muscle through targeted physical training so accommodation returns toward normal and myopic refractive error is reduced. VR can play a role here: because VR displays present virtual images at particular virtual distances and depth ranges, they can guide ocular focus and eye movements, providing exercise for the ciliary muscle and potentially contributing to myopia control.
Experimental Findings
To assess VR’s effects on children’s vision, the Advanced Imaging Innovation Center collaborated with Beijing Institute of Technology and other institutions in an experimental study using the professional-grade HTC Vive headset, which was among the leading headsets available in the Chinese market at the time. The published report indicated that several children who used the HTC Vive for one hour showed stable visual acuity and, in some cases, small improvements.
The experiment recorded an effective virtual image distance for the tested VR device of up to 1.7 m. A relatively distant virtual image can elicit accommodative responses from the eye’s lens, which may be beneficial for vision recovery. The researchers emphasized, however, that positive effects are contingent on selecting VR products with appropriate virtual image distance design and maintaining correct usage habits; otherwise, adverse effects are possible.
Key Technical Factors
Three technical factors influence whether a VR product is likely to be helpful: virtual image distance, refresh rate, and latency.
Virtual image distance: VR images are virtual, and the apparent image distance relative to the eye matters. Some consumer VR devices prioritize immersion by placing virtual images very close, at about 25–50 cm, which can induce visual fatigue after prolonged viewing. Higher-quality VR products set a farther virtual image distance, encouraging the eye to refocus and thereby exercising the ciliary muscle. For example, the HTC Vive’s measured virtual image distance is approximately 1.7 m.
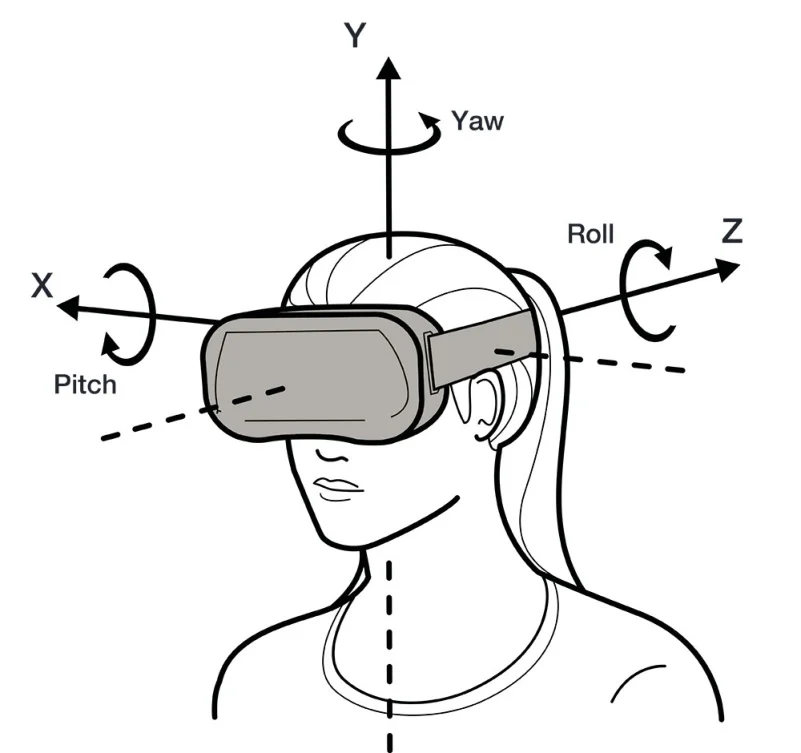
Refresh rate and latency: Refresh rate refers to how often the display is redrawn. Higher refresh rates produce more stable and clearer images, reducing strain on the eyes. Higher refresh rates also help reduce latency. Latency is the time from a user movement to the corresponding update on screen; long latency can cause discontinuities, judder, or ghosting, leading to dizziness and visual fatigue. Therefore, high refresh rates and low latency are important for minimizing adverse visual effects.
Product Selection Considerations
Some low-cost VR headsets on the market lack features such as interpupillary distance adjustment and object distance calibration; prolonged use of these devices can cause eye alignment problems and potentially permanent damage. Professional headsets such as Oculus Rift and HTC Vive typically use higher-quality optics and undergo more extensive design and testing. These devices tend to have higher-resolution displays, higher refresh rates, and lower latency, which reduces motion sickness and visual fatigue. When evaluating VR headsets, attention should be given to virtual image distance, lens quality, refresh rate, and latency.
Clinical Application
VR-based vision therapy systems have been developed and applied clinically. For example, a VR-based eye treatment system from Vivid Vision has been used by thousands of patients with visual disorders, producing measurable improvements. Work is also underway to develop consumer or home-use versions for platforms such as Oculus Rift, HTC Vive, and Gear VR to enable at-home treatment protocols.
Conclusion
VR technology offers a potential supplementary approach for myopia management by providing controlled accommodative and oculomotor stimuli. Positive outcomes depend on appropriate device design, correct usage patterns, and clinical validation. In contexts where electronic device use is difficult to eliminate, VR-based interventions may represent an option to combine visual training with controlled digital experiences. Further rigorous clinical studies are required to establish standardized protocols and long-term safety.
 ALLPCB
ALLPCB